Effective heart failure treatment relies on early diagnosis, management of comorbidities and a range of medical and interventional therapies. Garden City Heart offers full-service heart failure care that bridges the hospital and outpatient settings.

In 2017, the American Heart Association predicted a significant increase in heart failure. According to their Jan. 25 news release, more than 8 million Americans would experience heart failure by the year 2030, up from approximately 6.2 million today. While those numbers do not look to be trending up at the rate the American Heart Association predicted, heart failure remains a significant threat.
Of those with heart failure, many will die. According to the CDC, 1 in 8 American deaths is linked to heart failure. In 2018 alone, nearly 380,000 death certificates mentioned heart failure as a contributing cause, and the chronic condition costs billions of dollars in healthcare expenses, missed work and prescription costs. However, appropriate treatment measures can significantly diminish the risk of death and threat of financial loss.
“Mortality from heart failure is worse than cancer and creates a significant amount of cost in terms of health care,” says Felix Oviasu, MD, FACC, FACP, FCCP, board-certified cardiologist at Garden City Heart and Diplomate of the American Board of Internal Medicine and Nuclear Cardiology Board. “With adequate medical management, we can improve heart failure morbidity and mortality. Patients feel better, clinically present better and have reduced symptoms.”
To achieve positive results, physicians and patients must first take appropriate action. As with most medical conditions, the first step toward managing heart failure is a discussion of troublesome symptoms with a primary or specialty provider.
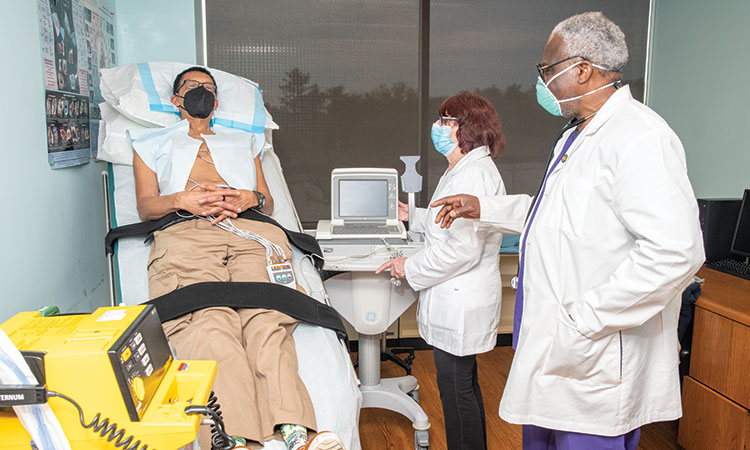
Connecting COVID-19 and Heart Failure
Since the beginning of the pandemic, the medical community has quickly developed an understanding of COVID-19, how it spreads and how to avoid and treat it. Despite this, “We don’t know everything about COVID-19,” says Felix Oviasu, MD, FACC, FACP, FCCP, board-certified cardiologist at Garden City Heart and Diplomate of the American Board of Internal Medicine and Nuclear Cardiology Board.
What Dr. Oviasu does know is that patients with COVID-19 may present with cardiac conditions, including myocarditis. In some cases, those presentations are significant enough to require hospitalization. Heart failure can also occur as a COVID-19 complication. Determining who will experience COVID-19-induced heart failure is no easy task, as it sometimes affects those who do not require hospitalization.
This increased incidence is not unexpected, Dr. Oviasu notes. As a virus, COVID-19 can directly affect the heart muscle. It can also set off an immune response that ultimately affects the heart muscle. This inflammation of the heart causes myocarditis. When severe, myocarditis can result in the development of a low ejection fraction and ultimately heart failure.
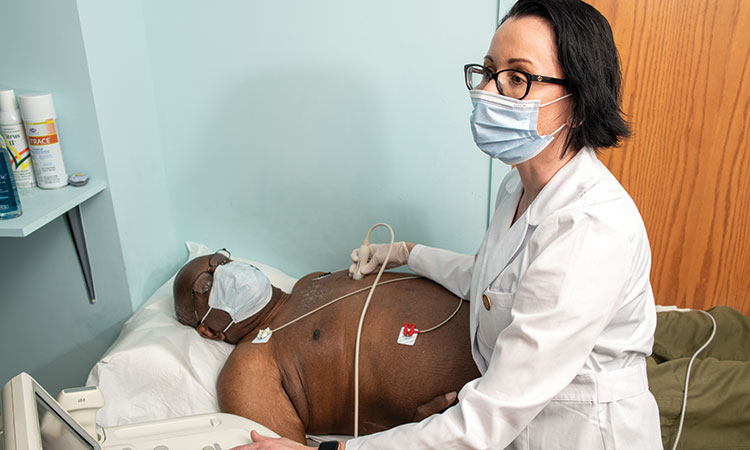
While anyone can experience such complications, certain individuals are at higher risk.
“Those with comorbidities are more likely to succumb to COVID-19 [and heart failure brought on by COVID-19],” Dr. Oviasu says. “And those with preexisting heart failure have an increased risk of mortality when infected with the virus.”
With this information, clinicians ought to be particularly protective of their patients with preexisting conditions, encouraging them to exercise extra caution to avoid infection.
Suspecting Heart Failure
Clinicians who suspect a patient is experiencing heart failure have an array of means to determine its presence. The first step to begin the diagnostic process is a thorough medical history. Topics to discuss with patients include existing medical conditions, family medical history, any medication therapy currently prescribed and the patient’s adherence to dosage and frequency recommendations.
Additionally, Dr. Oviasu says, providers ought to investigate any symptoms that potentially indicate heart failure. These wide-ranging symptoms arise from the heart’s inability to pump adequate blood throughout the body’s organs.
Symptoms that may indicate heart failure include the following:
Coughing that is persistent. The patient’s cough may or may not produce white or blood-stained mucus.
Edema in the abdomen or lower extremities. Swelling in the feet, legs or ankles and subsequent weight gain is a telltale sign of heart failure.
Feeling breathless, often with activity. This lack of oxygen can also occur when at rest or while sleeping. It may force an individual to sit upright in bed in the middle of the night to improve breathing.
Feelings of fatigue. Walking and exercise can become difficult due to heart failure. Such tiredness complicates the patient’s ability to perform activities of daily living and reduces overall quality of life.
Loss of appetite. Heart failure patients often struggle to eat. This may be due to feelings of fullness, which may be accompanied by nausea.
Mental acuity deficits. Heart failure can reduce an individual’s mental strength and stamina. With heart failure, the patient may experience atypical memory difficulty, confusion and other mental impairments.
Palpitating heart. A failing heart is constantly attempting to catch up and perform its duty properly, compensating for the heart’s lost pumping ability. As it does this, the patient may experience a noticeably rapid heart rate.
Should such symptoms be present, an in-depth examination helps determine the presence or absence of heart failure. Following a physical examination and discussion of medical history, the clinician may perform a series of ancillary tests to uncover heart failure.
Ancillary tests for heart failure include blood tests, chest radiography, electrocardiography and echocardiography. Through these testing modalities, clinicians can identify congestion in the lung or heart or a cardiac gallop due to abnormal function of the heart.
An abnormal electrocardiogram is also diagnostically significant, as it may suggest a previous myocardial infarction. Additional testing, such as echocardiogram, reveals the patient’s ejection fraction. At the same time, this exam can provide evidence of mitral or aortic valve regurgitation, all of which may relate to heart failure.
If it’s unclear whether the patient is experiencing active heart failure, Dr. Oviasu recommends caution.
“If the patient is out of heart failure, you can use noninvasive tests in terms of a nuclear exercise stress test,” he says. “Or you go directly for a cardiac angiogram.”
The decision to proceed directly to a cardiac angiogram comes with immediate benefit, Dr. Oviasu says. It allows the cardiologist to visualize the heart’s blood vessels and determine whether the patient is experiencing significant coronary artery disease (CAD). If so, that CAD might contribute to a patient’s symptoms. This important finding helps guide treatment and further ensures the preservation of the patient’s health and safety.
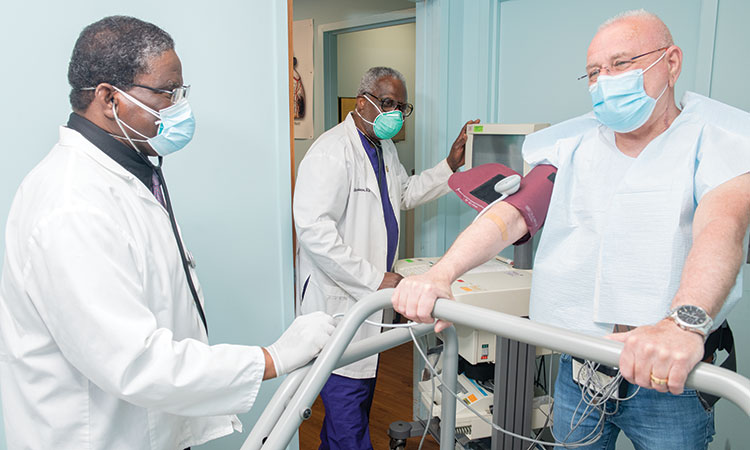
The Role of Hypertension
A variety of lifestyle choices and genetic problems culminate in a heart failure diagnosis. Among them, one stands out.
“Across the world,” Dr. Oviasu says, “hypertension is one of the biggest causes of heart failure.”
With untreated hypertension, the heart weakens over time. This weakened heart muscle produces a lowered ejection fraction, a primary origin of heart failure. Though hypertension is often the result of unhealthy habits, a lack of treatment for the disease, according to Dr. Oviasu, has another root.
“Hypertension often goes untreated because of social issues,” he says. “Some patients don’t have access to care, particularly within minority groups.”
Additionally, among those with access to care, there is some hesitancy to comply with prescribed medication for hypertension. One reason is hypertension medication comes with certain risks of its own. The most dreaded is the risk of a lowered libido. Among those with hypertension, many patients value their sexual desire over any risk of high blood pressure. Therefore, they do not take medication as prescribed.
Unfortunately, this lack of therapeutic management has significant complications. Hypertension can cause hypertrophy. This enlarging of the left ventricle can lead to CAD. When it does, CAD may result in heart failure. In fact, hypertrophy is the most common cause of heart failure in America.
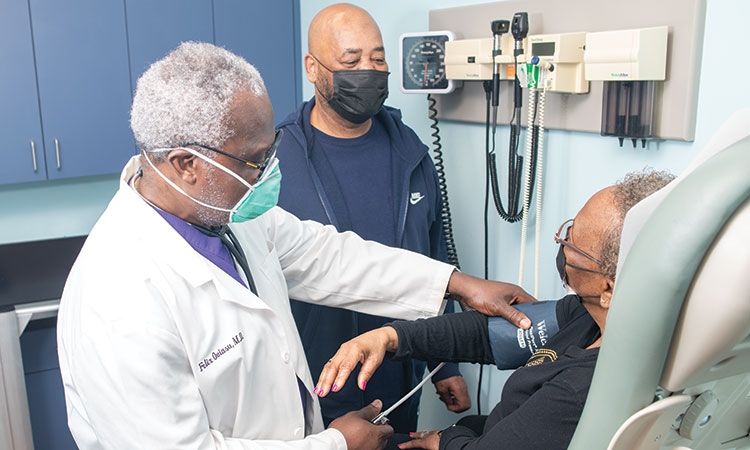
Additional Risk Factors: Diabetes
Dangerous as it is, hypertension is only one risk factor for heart failure. Another cause is diabetes. With diabetes, however, diagnosis of heart failure can be particularly difficult. Patients who have diabetes do not necessarily present with traditional angina symptoms. Therefore, they may not receive an accurate diagnosis at an early heart failure stage. As a result, many do not receive appropriate, aggressive heart care until they have experienced damage to the heart muscle.
Understanding this and taking appropriate action early may play a role in stopping heart failure from worsening over time. In some cases, recognizing the right signs may halt the development of heart failure altogether.
“It’s important that cardiologists treat risk factors aggressively — especially hypertension,” Dr. Oviasu says. “They should also look for early signs that might contribute to heart failure through noninvasive testing.”
If a patient presents with a low ejection fraction, the cardiologist is responsible for determining whether CAD is or is not present. An ejection fraction less than 50 should raise suspicion. In most cases, hypertension, CAD or ischemic heart disease is to blame. However, other problems may be present. For instance, the patient may have abused alcohol, which can affect ejection fraction and cause heart failure. In some cases, untreated sleep apnea can lead to atrial fibrillation or heart failure. Treating the underlying condition often brings symptomatic relief for heart failure patients.

Diagnostic Order of Operations
At Garden City Heart, a suite of diagnostic tests provides a full picture of a patient’s heart health and helps detect heart failure. Patients who come to Garden City Heart may undergo the following procedures:
Electrocardiogram. This test shows the heart’s rhythm and electrical activity, which may indicate a previous heart attack, arrhythmia or thickened left ventricle.
Echocardiogram. This standard ultrasound test reviews the heart’s ability to pump blood through the body. It is the most accepted manner of assessing the heart’s ejection fraction, which helps identify the presence of heart failure.
Nuclear exercise stress test. With this test, clinicians seek for ischemia, which may suggest the cause of a patient’s heart failure in terms of ischemic heart disease.
Holter monitor. This device provides evidence that a patient is experiencing the persistent rapid heart rate of atrial fibrillation, which can contribute to heart failure, or an irregular heart rate, such as tachycardia, which can be the result of heart failure.
Though these tests are typically performed in succession, they are not always indicated.
“If someone presents with unstable angina — they’re having chest pain at rest and it is progressively worsening — you may suspect that individual has significant ischemic heart disease,” says Felix Oviasu, MD, FACC, FACP, FCCP, board-certified cardiologist at Garden City Heart and Diplomate of the American Board of Internal Medicine and Nuclear Cardiology Board. In that case, he says, “You may go directly to a coronary angiogram without undergoing a stress test or other tests, because you believe the risk of noninvasive testing will be too high.”
Effective Therapies for Heart Failure
Today, a number of medical therapies are available to effectively manage heart failure. This is a great advance from years past. When Dr. Oviasu began practicing three decades ago, there were limited options. At that time, diuretics and digitalis were the treatments of choice. In fact, they were the only approved treatments for managing heart failure. Thirty years ago, accepted best practices recommended against the use of beta blockers for heart failure. Medical schools actively taught against using the medication, as the research of that day suggested beta blockers exacerbated heart failure symptoms.
A few years later, groundbreaking research found the exact opposite. Instead of worsening heart failure, beta blockers were found to have a positive effect. Researchers determined beta blockers improved the two major benchmarks of medical care: morbidity and mortality rates. Their use has since become standard practice within the heart failure patient population.
Soon after beta blockers became a standard of care, landmark studies found benefit in another medication: angiotensin-converting enzyme (ACE) inhibitors. Research found that this medication helps people with fully developed heart failure or post-myocardial infarction with low ejection fraction. Those prescribed ACE inhibitors enjoyed longer survival. Angiotensin receptor blockers were also shown in studies to improve heart failure patient outcomes. As researchers continued developing new treatment options, patients benefited.
“With time, there have been significant improvements in the treatment of heart failure,” Dr. Oviasu says. “ACE inhibitors have been key in terms of the improvement they’ve provided.”
However, he is quick to admit that the overall improvement in outcomes for those with heart failure is not due to a single advance. Rather, “It’s due to a combination of these medications.”
In addition to ACE inhibitors and beta blockers, other medical therapy increases success rates of heart failure management. This includes a diuretic and more recently sodium-glucose cotransporter 2 inhibitors (SGLT2 inhibitors). Originally developed to aid in glycemic control among adults with Type 2 diabetes, SGLT2 inhibitors earned FDA approval in 2020 as an additional method of managing heart failure.
For best results, Dr. Oviasu recommends not a single medication, but rather a judicious mix of these four approved medications. According to Dr. Oviasu, patients who can tolerate a combination of beta blockers, ACE inhibitors, SGLT2 inhibitors and a diuretic have an increased likelihood of improvement in their heart failure symptoms.
Living with Heart Failure
Heart failure is rarely curable. Treatment aims to address symptoms. With appropriate therapy, the patient experiences relief from troublesome symptoms, and as symptoms are reduced or eliminated, the individual can enjoy a full life that includes proper heart failure management.
“Most of the time, treatment is successful, and the patient feels better,” Dr. Oviasu says.
This improvement is dependent upon the initial symptoms. Those with leg swelling experience a reduction in swelling. Breathing becomes easier, which empowers the patient to walk longer distances without shortness of breath. The patient can often re-engage in activities of daily living that were once set aside as too demanding due to breathing difficulties or a lack of energy. Chest pain is reduced. Patients can again lie flat on their backs without struggling to breathe.
These improvements occur as the patient’s ejection fraction increases. As their ejection fraction nears the 50% goal, patients experience renewed energy. For some, this is the first bit of normalcy they have experienced in months or even years — all because of proper heart failure management.

Privileged Admissions
When heart failure requires more than lifestyle modifications and medication therapy, inpatient hospital care may be necessary. Fortunately, Felix Oviasu, MD, FACC, FACP, FCCP, board-certified cardiologist at Garden City Heart, Diplomate of the American Board of Internal Medicine and Nuclear Cardiology Board, has admitting privileges at two of the area’s most respected hospitals for heart care — St. Francis Hospital & Heart in Roslyn, New York, and North Shore University Hospital in Manhasset, New York.
Outpatient, Inpatient Care
In most cases, heart failure patients receive treatment in an outpatient setting. At Garden City Heart, Dr. Oviasu diagnoses a patient’s heart condition and then prescribes medication. The patient then returns home and self-administers the medication. Dr. Oviasu provides ongoing oversight in collaboration with the patient’s family physician.
Should a more invasive treatment become necessary, inpatient intervention is available. Dr. Oviasu has admitting privileges at Long Island’s major heart hospitals, allowing him to admit patients to the facility that is best able to meet their specific needs.
Inpatient procedures for heart failure may include cardiac catheterization and angiography, which Dr. Oviasu performs. Severe cases may indicate a need for heart transplant or other significant surgical intervention. Through Garden City Heart, patients transition seamlessly through every aspect of their care.
“I have access to excellent local surgeons [who perform] coronary bypass surgery, valvular surgery, and electrical studies or interventions,” Dr. Oviasu says. “[By partnering with these other experts], I can guide patients to the optimal result for their heart failure.”

For more information, please visit gardencityheart.com.
Source: MD News April 2022, Long Island Edition
